
25 Reasons Why People Use Drugs
Learn about all most common reasons why people use drugs and about the most effective addiction treatments at our We Level Up Lake Worth FL facility.

Learn about all most common reasons why people use drugs and about the most effective addiction treatments at our We Level Up Lake Worth FL facility.

Mixing Suboxone and cocaine can lead to severe physical and psychological risks. Learn all about the dangers from our We Level Up Lake Worth FL experts.

Is Ecstasy a Depressant or Stimulant? Discover the effects and importance of awareness. Level Up Lake Worth offers treatment!
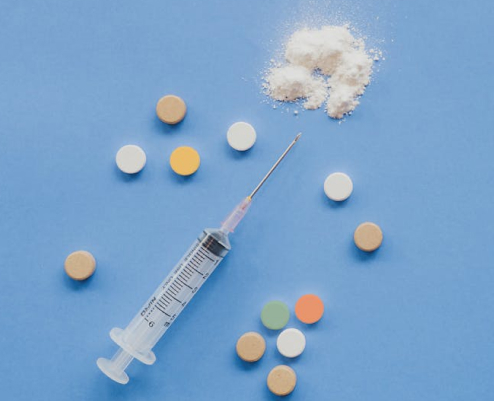
Heroin alone is an addictive substance. When laced with fentanyl, another opioid type, it becomes even stronger. In fact, fentanyl…

Ecstasy is a well-known illicit party drug, but many might not know what drugs are in ecstasy. Police confiscation in…

Discover the difference between cocaine and heroin, including treatment options at We Level Up Lake Worth in Florida. Contact us today!

The dangers of using a lean drink can quickly tear apart families and ruin lives without warning. This mixture often…

In Florida, more and more people are using fentanyl and xylazine together. These drugs are dangerous even on their own.…

Doctors often prescribe Xanax to assist people who have problems like intense worry or fear that comes from anxiety or…

A person's life can be profoundly impacted by chronic pain. It may have an effect on every aspect of your…

Not all US states have legalized marijuana (or, more colloquially, weed). Still, it seems that this partial legalization of the…

Prescription medicine can help people feel better. Doctors give these medicines to treat pain, anxiety or sleep problems. When used…
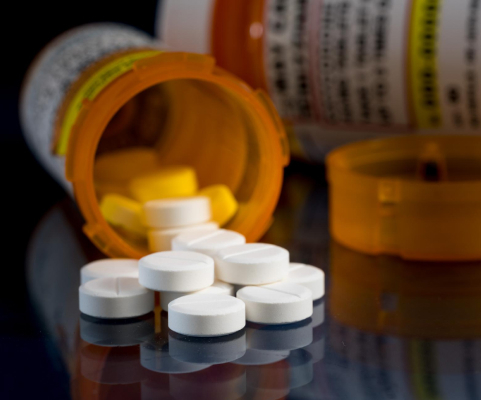
As a result of the epidemic of opioid addiction, overdoses, and fatalities it has created, the opioid crisis has been…

Is Adderall Addictive? Adderall addiction has become a serious public health concern, with many individuals dependent on the drug.

The serious and potentially harmful effects of combining Azithromycin and alcohol (azithromycin alcohol) are the reason for the warnings against alcohol consumption while taking Azithromycin. An increased risk of liver damage and toxicity is associated with taking Azithromycin and alcohol consumption.

Adderall Addiction Signs. Increased focus, energy, and productivity are common factors in substance abuse. Adderall can cause addiction and dependence on the user if it is taken without a doctor’s prescription or in a manner not recommended by medical professionals.

Even if you’ve never used gabapentin personally, you likely know someone who has. Initially created If you or your loved…

Many people ask, is addiction a disease? This question is very important. It helps us understand how to treat people…
Veins are a vast and intricate network of blood vessels located throughout every inch of the body. They are tasked…
Gabapentin is a medicine that doctors use to help with nerve pain, seizures, and sometimes anxiety. When it is used…